I have been diagnosed with a genetic heart condition known as LQTS (Long QT Syndrome) which is a rare inherited heart condition in which delayed repolarization of the heart following a heartbeat increases the risk of cardiac arrest.
The condition is named because of the appearances of the electrocardiogram (ECG/EKG), on which there is prolongation of the QT interval.
In May of last year (2013), I was at a routine physical and my doctor at the time thought he could hear a heart murmur, which can be harmless but nonetheless I was sent for a cardiac ultrasound at LHSC just to make sure.
The Ultrasound was 100% clear and the ”sound” he was hearing was chalked up to be just very strong heart valves. I met with a cardiac specialist right after the ultrasound because he had noticed something odd with my ECG. The doctor explained to me that my ultrasound was fine but there was a discovery of a different issue.
The doctor noticed that my QT wave was very long, so long that it was startling to him. Most people that have a pronounced QT wave of this length have had an “episode” in their life of fainting, head rushes or sudden death.
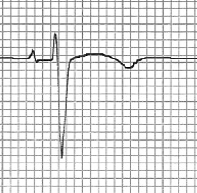
My wave below shows it quite clearly in the large long arch trailing at the end of the T wave. I am not sure of the measurement on this ECG but for example 400ms is considered long in males and mine was over that (600ms).
LHSC sent my blood away for genetic testing because there are some genes that have been discovered and from that different “types” of LQT have been medically documented.
My test came back positive for LQT3.
The LQT3 type of long QT syndrome involves mutation of the gene that encodes the alpha subunit of the sodium ion channel. This gene is located on chromosome 3p21-24, and is known as SCN5A (also hH1 and NaV1.5). The mutations involved in LQT3 slow the inactivation of the sodium channel, resulting in prolongation of the sodium influx during depolarization. However, the mutant sodium channels inactivate more quickly, and may open repetitively during the action potential.
I was shocked and upset about the whole thing as you can imagine because the number one thing not to do is compete in competitive sports. After doing a ton of research that night on the internet I came across SADS, the Canadian Sudden Arrhythmia Death Syndromes (SADS) Foundation, a registered Canadian charity and the only patient advocacy group in Canada dedicated to supporting families affected by inherited cardiac rhythm disorders.
I contacted them and a wonderful lady named Pam Husband answered all of my questions and suggested that I get a referral to the Peter Monk Cardiac Clinic in Toronto if possible. Her recommendation has proved to be invaluable because it was the missing link for me.
Dr. Danna Spears was the name Pam gave me, telling me that she was one of the Canadian leaders studying LQTS and Toronto is not that far from London so I thought lets go for it.
I scheduled a follow up with my family doctor, but to my surprise I found out he was leaving his practice to go back and teach medicine no longer continuing to be a family physician. He asked me if there was anything he could do for me before he left medication wise but all I asked for was a referral to the clinic in Toronto. He felt that is was a good idea to get a second opinion from a specialist and sent off the referral forms.
After a few months of cat and mouse and one lost referral form but I finally got scheduled an appointment for February 2014 at the Peter Munk Cardiac Centre.
This was all happening at an inconvenient time in my life because I was training regularly and as it turns out qualifying to go to worlds for Sprint Distance Duathlon. Mentally from May to June I was not myself because of the stress of this whole thing but I managed nonetheless to push though a qualifying event on my birthday June 1st, 2013 – Belle River Duathlon and secured my spot on the Canadian Duathlon Team for 2014.
After that race I was able to take a step back and recap all that had happened over the past few months realizing that this was not something I was mentally going to let get to me. Continuing with my racing with this new mental attitude I had a great summer of PB’s.
I knew until I saw the specialist there was nothing I could do so I just didn’t change anything in my life. I refused to take any suggested medications and decided that since I was not experiencing any symptoms or having any “episodes” then why change anything. “If something is working adequately well, leave it alone.”